Current Management of Type 2 Diabetes Mellitus in Primary Care Clinics in Korea
Article information
Abstract
Background
This study investigated the overall status of diabetes control and screening for diabetic microvascular complications in patients with type 2 diabetes mellitus attending primary care clinics in Korea.
Methods
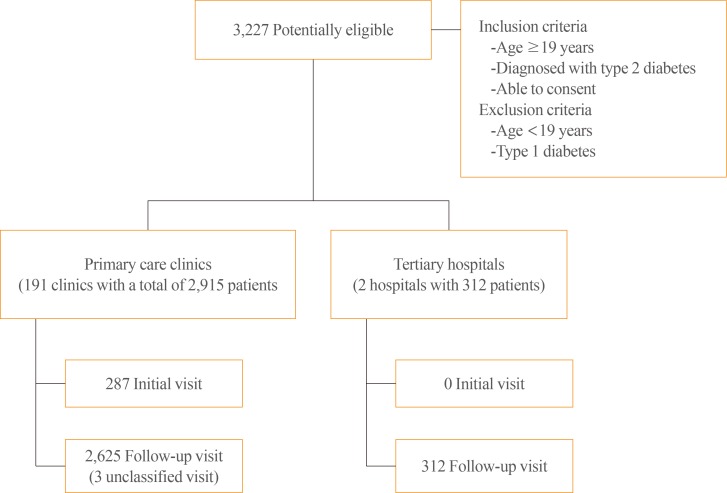
In this cross-sectional observational study, 191 primary care clinics were randomly selected across Korea from 2015 to 2016. In total, 3,227 subjects were enrolled in the study.
Results
The patients followed at the primary care clinics were relatively young, with a mean age of 61.4±11.7 years, and had a relatively short duration of diabetes (mean duration, 7.6±6.5 years). Approximately 14% of subjects had diabetic microvascular complications. However, the patients treated at the primary care clinics had suboptimal control of hemoglobin A1c levels, blood pressure, and serum lipid levels, along with a metabolic target achievement rate of 5.9% according to the Korean Diabetes Association guidelines. The screening rates for diabetic nephropathy, retinopathy, and neuropathy within the past 12 months were 28.4%, 23.3%, and 13.3%, respectively.
Conclusion
The overall status of diabetes management, including the frequency of screening for microvascular complications, was suboptimal in the primary care clinics. More efforts should be made and more resources need to be allocated for primary care physicians to promote adequate healthcare delivery, which would result in stricter diabetes control and improved management of diabetic complications.
INTRODUCTION
The prevalence of type 2 diabetes mellitus (T2DM) continues to rise and is projected to increase to 592 million in 2035 worldwide [12]. Unfortunately, Korea is not an exception; the prevalence of diabetes is steadily increasing and a recent study revealed that about 4.8 million Korean adults (13.7%) have diabetes [3]. Both microvascular and macrovascular complications develop quite commonly in patients with diabetes, and cause significant morbidity and mortality [45].
Trials investigating diabetes control and complications have shown that intensive glycemic treatment effectively delays the onset and progression of diabetic microvascular complications in type 1 diabetes [6], and similar findings were noted in patients with T2DM [7], with benefits extending beyond the period of intervention [89]. Despite strong evidence of the benefits of tight glycemic control, an analysis of data from the 2014 Korea National Health and Nutrition Examination Survey (KNHANES) indicated that more than 50% of adults diagnosed with diabetes in Korea failed to achieve a hemoglobin A1c (HbA1c) level below 7%, a result similar to that found in the USA [1011]. A few studies have demonstrated that the overall diabetes management in patients who attended primary care clinics was less optimal than that of patients followed at secondary or tertiary hospitals [121314], but there is a paucity of data comparing primary care to secondary or tertiary care following the release of the Korean Diabetes Association (KDA) clinical practice guidelines.
In response to the increasing prevalence of non-communicable diseases (NCDs), the Korean government introduced a clinic-centered NCD management policy in 2012, which focused on strengthening the role of primary care clinics as an important source of outpatient care for NCDs [15]. According to the Health Insurance Review & Assessment Service, approximately 60% of patients with diabetes visited primary care clinics for management of diabetes in 2017 [16]; however, very few studies have examined the rate of adherence to the KDA guidelines in primary care clinics. The primary aim of this study was to examine the current status of overall diabetes management, including the screening rate for microvascular complications, among patients with T2DM visiting primary care clinics. The secondary aim was to compare the findings from primary care clinics to those from two tertiary hospitals in Seoul.
METHODS
Study design and population
A total of 191 primary care clinics were randomly selected across Korea, from which 2,915 patients with T2DM were enrolled in this study from January 2015 to September 2016 (Fig. 1). To maximize the generalizability of the results, the subjects were selected by random sampling from 16 cities and provinces (seven special and metropolitan cities including Seoul, Busan, Daegu, Incheon, Gwangju, Daejeon, and Ulsan) and nine provinces (Gyeonggi-do, Gangwon-do, Chungcheongbuk-do, Chungcheongnam-do, Jeollabuk-do, Jeollanam-do, Gyeongsangbuk-do, Gyeongsangnam-do, and Jeju provinces) across Korea. The regional distribution of the enrollees was similar to that of the entire Korean population, as in the 2017 Korean Population Census [17]. As a secondary objective of our study, we compared primary care clinics with tertiary hospitals by analyzing data from 312 patients with T2DM who attended tertiary hospitals for diabetes management, at Severance Hospital in the northern part of Seoul and Gangnam Severance Hospital in the southern part of Seoul (the total number of outpatient visits for diabetes management per year are 30,879 patients/year and 16,155 patients/year at Severance Hospital and Gangnam Severance Hospital, respectively). Among all patients who met both inclusion and exclusion criteria, those who consented were enrolled in the study consecutively. The inclusion criteria of the study were patients with T2DM who were ≥19 years old and were willing to provide consent. Patients with type 1 diabetes and patients who were <19 years old were excluded. A diagnosis of type 1 diabetes were made if one of the following conditions was present; fasting C-peptide ≤0.6 ng/mL, postprandial 2-hour C-peptide ≤1.8 ng/mL, anti-glutamic acid decarboxylase antibody positivity, anti-insulin antibody positivity, or antiislet cell antibody positivity. Atherosclerotic cardiovascular disease (ASCVD) was defined as a previous history of stroke, ischemic heart disease, or peripheral vascular disease. Data, including laboratory assessments, were collected on the day of the outpatient clinic visit and were recorded in a pre-formulated case report by the physicians. The study protocol was approved by the Institutional Review Board of Severance Hospital, and written informed consent was obtained from all participants (IRB no. 4-2014-0904 and IRB no. 3-2014-0270).
Anthropometric and biochemical measurements
Data collected from the patients included demographic characteristics, past medical history, duration of diabetes, smoking history, as well as any history of diabetic vascular complications within the 12 months before enrollment. The treatment modalities of diabetes were classified as diet only, oral hypoglycemic agents (OHAs) alone, insulin alone, or a combination of insulin and OHAs. For those who were current smokers or had any history of smoking, data on whether they were ever offered smoking cessation intervention during previous encounters with the physicians were also gathered.
Each patient's height, weight, waist circumference, and blood pressure (BP) were measured and participants were also asked about the date and modality of BP measurements (i.e., digital method or analog method). Hypertension was defined as a BP ≥140/90 mm Hg or taking antihypertensive medication(s).
Data on when the laboratory assessments were done were also collected, as well as the types of blood tests (capillary or plasma blood test) and the frequency and type of glycemic assessments (fasting glucose, random glucose, or HbA1c). To evaluate dyslipidemia, data were collected on the types of lipid tests (total lipid panel or partial lipid profile) in the 12 months before enrollment. Screening for microvascular complications was considered to have been done if there were records of any of the following: fundus eye exam, spot urine test for albumin-to-creatinine ratio or 24-hour urine test, monofilament test, pinprick test, ankle reflex test, nerve conduction test, or a referral to a specialist within the previous 12 to 24 months. Microalbuminuria and overt proteinuria were defined as a random urine albumin-to-creatinine ratio between 30 and 300 mg/g and above 300 mg/g, respectively. The prevalence of retinopathy, nephropathy, neuropathy, ischemic heart disease, cerebrovascular disease, and peripheral artery disease was investigated based on the patient's past medical history. The optimal targets were defined as HbA1c <6.5% for blood glucose, <140/85 mm Hg for BP, and low density lipoprotein cholesterol (LDL-C) <100 mg/dL for the blood lipid profile [18]. For those with ASCVD, BP <130/80 mm Hg and serum LDL-C <70 mg/dL were defined as the optimal targets according to the KDA treatment guideline for diabetes 2019 [18].
Statistical analysis
We used SPSS version 20.0 (IBM Corp., Armonk, NY, USA) for the statistical analysis and considered P values <0.05 to indicate statistical significance. Continuous variables with a normal distribution were presented as mean±standard deviation (SD), and categorical variables as absolute numbers (percentages). The Student t test, chi-square test, and Fisher exact test were used to test the statistical significance of differences between mean values.
RESULTS
General characteristics and diabetes control status of the study population
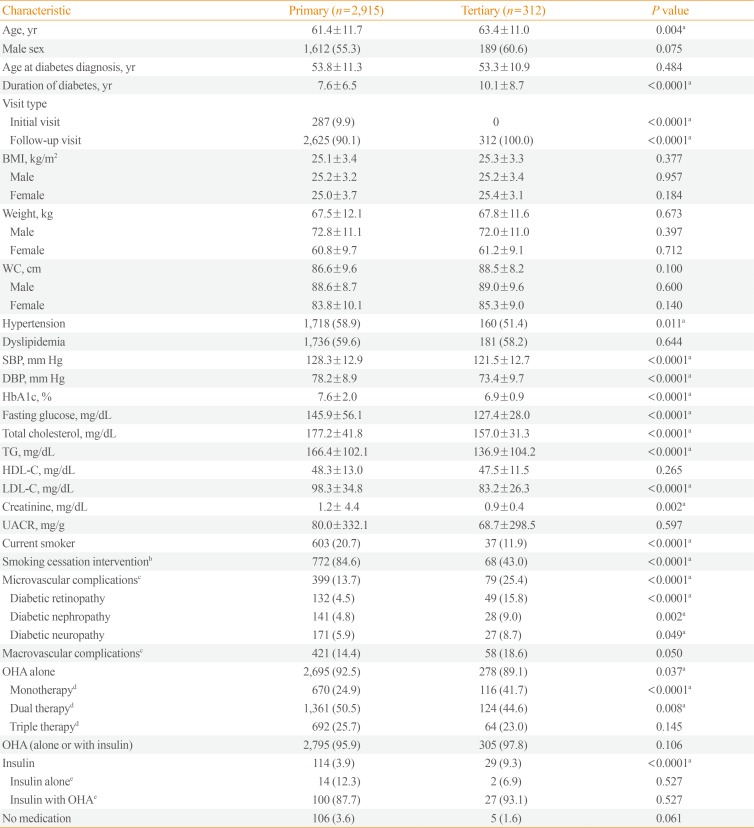
The mean age of the subjects in the primary care setting was 61.4±11.7 years and the mean duration of diabetes was 7.6±6.5 years, with a mean HbA1c of 7.6%±2.0%. Approximately two-thirds of the patients had concomitant hypertension and dyslipidemia, with suboptimal control of blood glucose, serum lipids, and BP (Table 1). The prevalence of diabetic microvascular and macrovascular complications were 13.7% and 14.4%, respectively (Table 1). Among the 2,915 patients with T2DM followed at primary care clinics, the majority of the patients were treated with OHAs (96%) and the most frequently prescribed OHA was metformin (84%), followed by dipeptidyl peptidase 4 (DPP4) inhibitors (65%) and sulfonylureas (41%) (Supplemental Table S1). The proportion of the patients prescribed OHAs was significantly higher than the insulin prescription rate of 4% (Table 1).
Screening rate for diabetic microvascular complications and metabolic target achievement rate
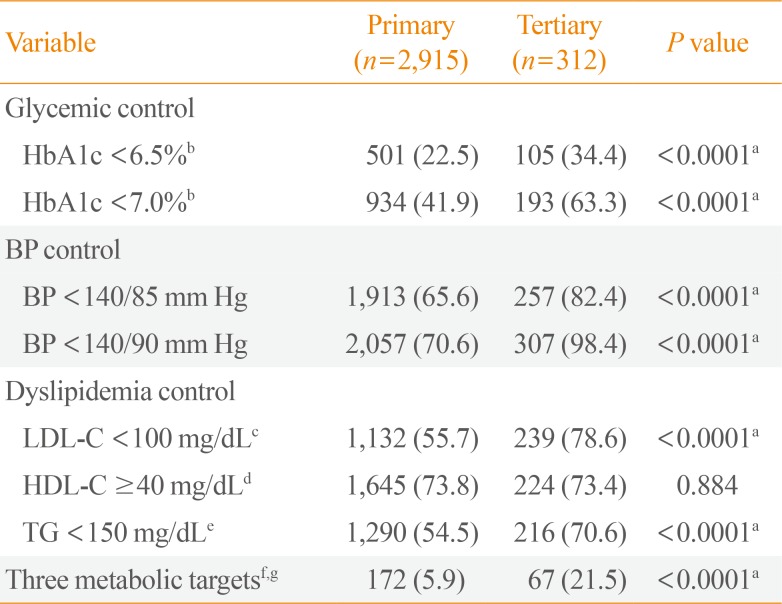
The overall prevalence of diabetic complications was significantly lower among the patients treated at primary care clinics than among those treated at tertiary hospitals (Table 1). The screening rates for diabetic retinopathy, nephropathy, and neuropathy within the past 12 months were 23%, 28%, and 13%, respectively, at primary care clinics (Table 2, Fig. 2). In other words, more than two-thirds of patients did not receive any screening tests in a year. Moreover, the proportion of the patients who achieved optimal metabolic targets (HbA1c, BP, and LDL-C) was only 5.9% among those followed at primary care clinics (Table 3). In a sub-analysis of those with ASCVD, the proportion of subjects who achieved the optimal BP and lipid profile targets (BP <130/80 mm Hg and LDL-C <70 mg/dL) was 26.4% and 16.6%, respectively (Supplemental Table S2).
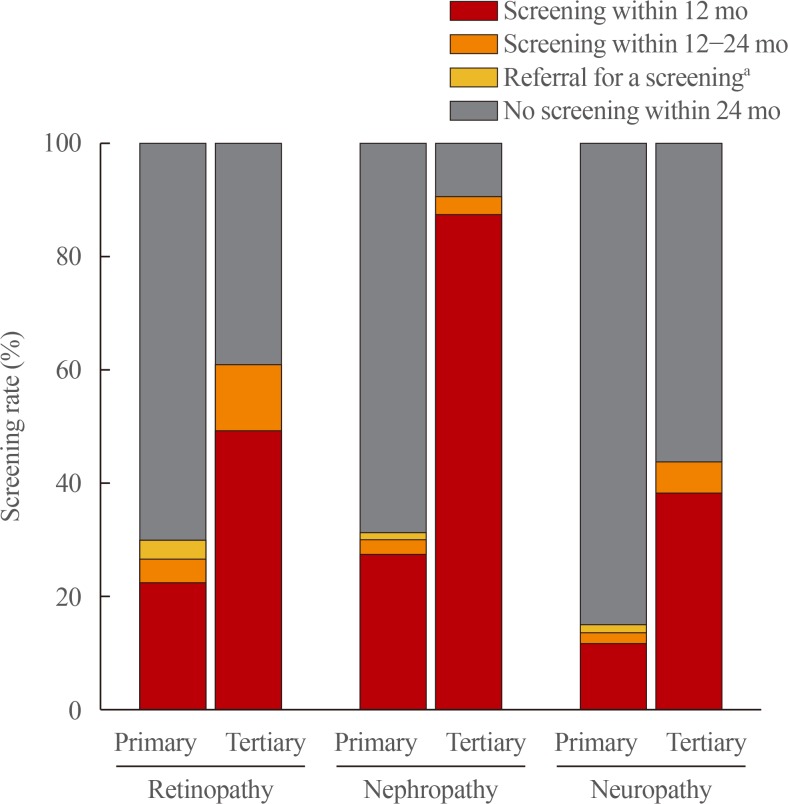
Comparison of the screening done for microvascular complications at primary care clinics versus the tertiary hospitals. aReferral for screening tests within 24 months.
Frequency and method of glucose, BP, and cholesterol monitoring
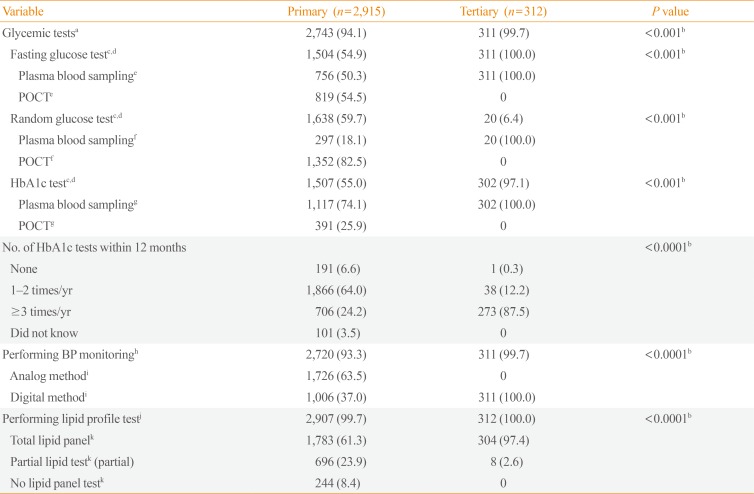
Although 95% of the subjects had at least one form of glycemic assessment (random glucose testing, fasting glucose testing, or HbA1c test), HbA1c testing was significantly underutilized at primary care clinics. Furthermore, two-thirds of the patients followed at primary care clinics only received HbA1c tests one to two times per year (Table 4).
For BP monitoring, 94% of the subjects had BP measurements taken on the day of their encounter at a primary care clinic, and the analog method was still preferred to assess BP. For lipid profile tests, the proportion of the subjects who had a total lipid panel test was significantly less at primary care clinics (Table 4).
Smoking status and counseling
Among the subjects who attended the primary care clinics, 20.7% were current smokers, and the majority of current smokers were offered smoking cessation education or counseling.
DISCUSSION
This study investigated the overall status of diabetes management in 2,915 patients with T2DM treated at primary care clinics in Korea, and found that most of the patients did not meet the current clinical practice guidelines recommended by the KDA. Only approximately 22.5% of the patients achieved the recommended level of glycemic control. These findings agree with those of previous studies of primary care settings that showed a high frequency of poor glycemic control [12]. Our data also demonstrate that a low proportion of patients received screening tests for microvascular complications, which clearly demonstrates a deficiency in the management of diabetes. Hence, more efforts and suitable measures need to be introduced to improve the care provided to patients with diabetes at primary care clinics in Korea.
The prevalence of T2DM and its complications continues to rise [101920]. In order to prevent diabetic microvascular and macrovascular complications, comprehensive management of diabetes is crucial. Despite the development of numerous new antidiabetic medications, the proportion of patients achieving target glycemic control (HbA1c <7% defined by the American Diabetes Association [ADA] guidelines) has plateaued in the United States since 2006 [11]. In Korea, the proportion of the patients achieving optimal glycemic control (i.e., HbA1c <7%,) continued to improve from 42.5% in 2005 to 44.9% in 2014 [10]; however, this proportion was significantly lower for patients treated at primary care clinics than for those treated at tertiary hospitals in our study (41.9% vs. 63.3%, P<0.0001). In other words, a large proportion of patients are still at a high risk of developing diabetic complications, particularly those who attend the primary care clinics.
There have been significant changes in the prescription patterns of antidiabetic medications following the introduction of DPP4 inhibitors in 2008. In 2002, sulfonylureas were the most commonly used antidiabetic medications for T2DM patients; however, the prescription rate for metformin has steadily increased, and metformin has been the most frequently prescribed antidiabetic drug since 2013, followed by sulfonylureas and then DPP4 inhibitors [19]. These changes are clearly reflected in the prescription patterns found in our study, where the most commonly prescribed dual combination was metformin and a DPP4 inhibitor. DPP4 inhibitors are readily used by many healthcare providers, including primary care physicians, because of their ease of use, fair glycemic control, neutral effect on body weight, and low hypoglycemia rate. However, the proportion of the subjects prescribed insulin was very low at primary care clinics. This may be partly due to the introduction of various antidiabetic agents, including DPP4 inhibitors, and a shortage of educational staff with expertise on insulin therapy at primary care clinics [12].
Both ADA and KDA guidelines recommend monitoring HbA1c at least biannually in patients with stable glycemic control and quarterly in patients who do not meet their treatment goals or who have changed medication [1821]. Despite steady improvements in the frequency of HbA1c monitoring since the introduction of a diabetes care quality assurance program [16], those managed at primary care clinics were infrequently tested for HbA1c [22]. Furthermore, consistent with previous reports [1622], random glucose testing using a portable glucometer was the most commonly used method for glycemic monitoring, most likely because of the lack of laboratory facilities at primary care clinics. This indicates that poor diabetes control in patients treated at primary care clinics may be related to less intensive and less frequent monitoring, despite shorter visit intervals.
Despite the recommendations on annual screening for diabetic microvascular complications contained in the KDA guideline [18], the screening rates for diabetic retinopathy, nephropathy, and neuropathy at primary care clinics were quite low. Previous studies have suggested that a lack of resources, such as limited access to facilities for screening tests for complications, and patients' socioeconomic status were associated with the frequency of diabetic screening tests [232425]. Similar findings were also noted in the Pittsburgh Epidemiology of Diabetes Complications study, in which it was found that receiving care from primary care physicians, instead of from diabetes specialists, was associated with lower preventive service utilization and poorer glycemic control [26]. Physicians' attitudes toward caring for diabetic patients can be another barrier, as some primary care physicians felt that the guidelines for reaching the goals were not clear and relied on their clinical experience when making decisions to screen [2427]. Moreover, they often faced administrative, time, and information constraints [27]. As preventive health care is the cornerstone of the primary and secondary prevention of diabetes complications, improving diabetes education for both patients and providers in primary care settings and establishing a system that allows easy referrals to specialists may improve the utilization of preventive services.
Moreover, a systemic program or a policy needs to be implemented by the government in order to improve and sustain the comprehensive management of diabetes at primary care clinics. It is necessary to introduce a compensation system based on the health outcomes of patients to encourage primary care physicians to participate more actively in the management of diabetes. For example, the introduction of non-monetary compensation systems, such as the Green Prescription Clinics, for clinics with excellent target achievement rates can drive voluntary quality improvement of primary care clinics.
There are some limitations of this study. First, this was a cross-sectional observational study, which did not allow us to monitor changes over time. Second, a total of 312 patients from two tertiary hospitals were enrolled for this study and used as comparators. However, the tertiary hospitals may have been primarily representative of the Gangbuk and Gangnam areas, whereas the primary endpoint of this study was to examine the current status of T2DM management at primary care clinics. Nevertheless, this is the first study to examine the current status of diabetes management in Koreans, especially with a focus on the frequency and method of follow-up tests and screenings for microvascular complications at primary care clinics.
In conclusion, despite steady improvements over the past decade, we found that the overall status of diabetes management, including the screening rates for complications, was still suboptimal in patients with T2DM who attended primary care clinics. Substantially more efforts and resources need to be deployed for primary physicians to improve their adherence to clinical practice guidelines and to deliver the most optimal healthcare in the primary care setting.
Notes
CONFLICTS OF INTEREST: This study was supported by a research grant from Ildong Pharmaceutical Co., Ltd. One of the co-authors, Jung Yoon Ha, is a current employee at Ildong Pharmaceutical Co., Ltd., but no potential conflict of interest was reported by the author.
AUTHOR CONTRIBUTIONS:
Conception or design: S.K., Y.L., J.Y.H., B.S.C.
Acquisition, analysis, or interpretation of data: D.H.S., S.K., Y.L., J.S.P., B.W.L., E.S.K., C.W.A., B.S.C.
Drafting the work or revising: D.H.S., S.K., B.S.C.
Final approval of the manuscript: D.H.S., S.K., B.S.C.
References
SUPPLEMENTARY MATERIALS
Supplemental Table S1
Hypoglycemic Medications for Glycemic Control
Supplemental Table S2
Metabolic Target Achievement Rate among Those with ASCVD