Cardiorenal Protection in Diabetic Kidney Disease
Article information
Abstract
Over the last 5 years there have been many new developments in the management of diabetic kidney disease. Glucagon-like peptide-1 receptor agonists (GLP-1 RA) and sodium-glucose cotransporter-2 (SGLT2) inhibitors were initially used for glycemic control, but more recent studies have now shown that their benefits extend to cardiovascular and kidney outcomes. The recent addition of data on the novel mineralocorticoid receptor antagonist (MRA) gives us another approach to further decrease the residual risk of diabetic kidney disease progression. In this review we describe the mechanism of action, key studies, and possible adverse effects related to these three classes of medications. The management of type 2 diabetes now includes an increasing number of medications for the management of comorbidities in a patient population at significant risk of cardiovascular disease and progression of chronic kidney disease. It is from this perspective that we seek to outline the rationale for the sequential and/or combined use of SGLT2 inhibitors, GLP-1 RA and MRAs in patients with type 2 diabetes for heart and kidney protection.
INTRODUCTION
Until recently, glycemic control, blood pressure management, angiotensin converting enzyme (ACE) inhibitors or angiotensin receptor blockers (ARB) were the only available strategies to prevent diabetic kidney disease (DKD) progression. Older glucose lowering therapies demonstrated efficacy with respect to achieving glycemic targets but lacked benefits for ‘hard’ kidney or cardiovascular (CV) outcomes [1]. Importantly, older glucose lowering therapies were also associated with potential harm related to heart failure (HF) hospitalizations with thiazolidinediones, as well as hypoglycemia and weight gain with therapies such as sulfonylureas and insulin [2].
Over the last 5 years, with the emergence of newer agents including sodium-glucose cotransporter-2 (SGLT2) inhibitors, glucagon-like peptide-1 receptor agonists (GLP-1 RA) and novel mineralocorticoid receptor antagonist (MRA), management of type 2 diabetes mellitus (T2DM) and DKD has since shifted away from a ‘glucose-centric’ focus towards one of ‘heart and kidney protection [3–5]. These newer agents have individually demonstrated CV and/or kidney benefits, and the combined use of these agents is particularly appealing due to potential mechanistic and clinical synergies [6]. Accordingly, our aim was to review the mechanisms and clinical benefits of these three classes of agents and outline the case for their combined use for heart and kidney protection in DKD.
SGLT2 INHIBITORS, CARDIOVASCULAR AND KIDNEY PROTECTION IN PATIENTS WITH T2DM
SGLT2 inhibition and mechanistic benefits
The precise mechanisms behind heart and kidney benefits of SGLT2 inhibitors are incompletely understood, though there are likely multiple complementary physiological effects [7,8]. Kidney protective mechanisms of SGLT2 inhibitors are commonly considered according to hemodynamic versus non-hemodynamic actions. By inhibiting proximal tubular sodium and glucose reabsorption, SGLT2 inhibitors increase distal sodium delivery to the macula densa and restore tubuloglomerular feedback, with the effect of decreasing intraglomerular pressure, shear stress, hyperfiltration and albuminuria [9–12]. The cardio-protective mechanisms linked with SGLT2 inhibitors also overlap with those associated with kidney protection. For example, beyond restoring glomerular pressure toward more normal physiological levels, hemodynamic effects in the systemic circulation induced by natriuresis restore relative euvolemia, lower blood pressure and arterial stiffness, and may contribute to improving cardiac preload and afterload [13,14].
Independent of hemodynamic effects, from a metabolic perspective, SGLT2 inhibitors promote glucosuria and modestly improve glycemic control [15,16]. The associated caloric loss also contributes to reductions in body weight by 2 to 3 kg on average, another traditional CV risk factor [15,17]. Glucosuria also enhances gluconeogenesis and ketogenesis, part of an SGLT2 inhibitor induced shift to a ‘fasting state.’ Ketogenesis is hypothesized to be a direct mediator of cardioprotection with SGLT2 inhibition since ketone bodies are an efficient energy source with the potential to improve myocardial energy dynamics and exert direct anti-inflammatory effects [18–20]. Alternatively, ketones may simply be an indirect biomarker of heart and kidney protection, with SGLT2 inhibitors activating ‘nutrient-deprivation pathways,’ leading to improved mitochondrial function and energy dynamics and less oxidative stress at the cellular level, with ketogenesis simply being a byproduct of this process [21–23]. These metabolic changes activated by ‘fasting state’ with SGLT2 inhibition may also ameliorate myocardial efficiency and hypoxia. SGLT2 inhibitors also inhibit myocardial sodium-hydrogen exchange, with hypothesized downstream benefits to cardiac hypertrophy and fibrosis [13]. SGLT2 inhibitors may also reduce energy requirements and hypoxia within proximal tubular cells, and may improve oxygen delivery by increasing hematocrit [24]. This, combined with their modulation of neurohumoral pathways and reduction of glucose entry into tubular cells, likely contributes to suppression of kidney hypoxia, inflammation, and fibrosis [25–29]. Finally, improvements in kidney function itself may indirectly improve cardiac function through reductions in sympathetic nervous system activation, systemic inflammation and chronic hypervolemia that characterize the chronic cardiorenal syndrome [30].
SGLT2 inhibition and clinical heart and kidney protection
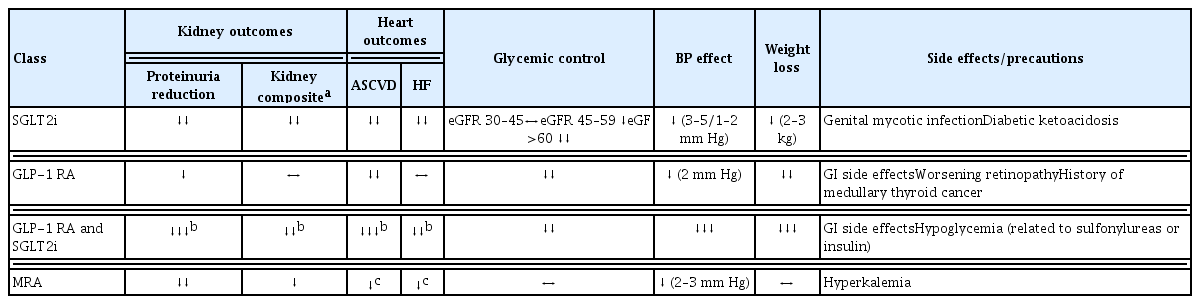
The heart and kidney protective effects of SGLT2 inhibitors were first demonstrated in three large cardiovascular outcome trials (CVOT) exclusively comprising participants with T2DM. The Empagliflozin Cardiovascular Outcome Event Trial in Type 2 Diabetes Mellitus Patients (EMPA-REG OUTCOME), Canagliflozin Cardiovascular Assessment Study (CANVAS Program) and Multicenter Trial to Evaluate the Effect of Dapagliflozin on the Incidence of Cardiovascular Events-Thrombolysis in Myocardial Infarction 58 (DECLARE-TIMI-58) trials included >34,000 patients and demonstrated significant reductions in the risk of major adverse cardiovascular events (MACE; composite of non-fatal stroke, non-fatal myocardial infarction and CV death) and/or hospitalization for heart failure (HHF) (Table 1 for a summary of effects) [31–33].
Secondary kidney composite outcomes were also consistently reduced across the three trials. In EMPA-REG OUTCOME, the kidney composite of albuminuria progression, doubling of serum creatinine, end-stage kidney disease (ESKD), or renal death was reduced by 39%, with consistent benefits across multiple subgroups including those with chronic kidney disease (CKD) at baseline [34]. In the CANVAS Program, the kidney composite (doubling of serum creatinine, renal replacement therapy or renal death) was similarly reduced by 47% (hazard ratio [HR], 0.53; 95% confidence interval [CI], 0.33 to 0.84) [35]. By design, DECLARE-TIMI-58 had the lowest CV risk cohort and the highest baseline mean estimated glomerular filtration rate (eGFR) of the three trials [32]. In this lower kidney risk cohort, dapagliflozin reduced the composite kidney endpoint, which included a more modest 40% decline in eGFR, ESKD or renal death, by 47% (HR, 0.53; 95% CI, 0.43 to 0.66) [13]. Risk reduction for CV outcomes was similar across baseline levels of kidney risk, aside from a lower HR in the impaired eGFR with albuminuria group [36]. Post hoc analyses have demonstrated that observed CV and kidney benefits in the original CVOTs were largely independent of glycemic lowering [37–40].
Two subsequent CVOTs were published in 2020. Cardiovascular Outcomes Following Ertugliflozin Treatment in Type 2 Diabetes Mellitus Participants with Vascular Disease (VERTIS-CV), which compared ertugliflozin with placebo showed non-inferiority in regards to its primary MACE outcome, as well as a 30% reduction in HHF [41]. For the key composite kidney endpoint, which used “doubling of serum creatinine” for the definition of significant kidney function loss, the impact of ertugliflozin was neutral [41]. However, as presented at the European Association for the Study of Diabetes 2020, with a more modest kidney endpoint comprised of a sustained 40% eGFR decline, a HR of 0.66 was observed (95% CI, 0.50 to 0.88) [42]. Additionally, when stratified by kidney risk in VERTIS-CV as determined by KDIGO risk categories, significant reductions in the HHF/CV death composite were observed in the moderate and high/very high risk categories (P=0.03 for interaction) [43].
In a second trial, Effect of Sotagliflozin on Cardiovascular and Renal Events in Patients With Type 2 Diabetes and Moderate Renal Impairment Who Are at Cardiovascular Risk (SCORED), a dual SGLT2 inhibitor and gastrointestinal SGLT1 inhibitor sotagliflozin was examined in patients with T2DM, CKD (eGFR from 25 to 60 mL/min/1.73 m2) and CV risk factors. Although the trial was stopped early due to a lack of funding, the trial investigators demonstrated a reduction in the primary cardiac composite endpoint (total number of deaths from CV causes, HHF and urgent visits for HF) of 26% (HR, 0.74; 95% CI, 0.63 to 0.88) [44]. While the composite kidney outcome including a 50% sustained decrease in eGFR was not statistically significant (HR, 0.71; 95% CI, 0.46 to 1.08), analyses with other kidney composites have not yet been published. Sotagliflozin also demonstrated safety and efficacy in patients with worsening HF in Effect of Sotagliflozin on Cardiovascular Events in Patients With Type 2 Diabetes Post Worsening Heart Failure (SOLOIST-WHF), although this trial was also stopped early due to insufficient funding [45].
Analyses of kidney outcomes in the original CVOTs prompted dedicated kidney outcome trials, of which two are completed: Evaluation of the Effects of Canagliflozin on Renal and Cardiovascular Outcomes in Participants With Diabetic Nephropathy (CREDENCE, NCT02065791) and A Study to Evaluate the Effect of Dapagliflozin on Renal Outcomes and Cardiovascular Mortality in Patients With Chronic Kidney Disease (DAPA-CKD, NCT03036150). These trials were both stopped early due to clinical benefit. CREDENCE included patients with an eGFR from 30 to 90 mL/min/1.73 m2 and a urine albumin-to-creatinine ratio (UACR) of 300 to 5,000 mg/g. The kidney specific outcome was a composite of ESKD, doubling of creatinine or death from a renal cause, and was reduced by 34% in the treatment group (HR, 0.66; 95% CI, 0.53 to 0.81) [46]. DAPA-CKD had broader inclusion criteria, dropping the eGFR and UACR cutoffs and including participants without diabetes. This trial enrolled 4,304 participants with an eGFR of 25 to 75 mL/min/1.73 m2 with a UACR of 200 to 5,000 mg/g. The primary outcome was a composite of a sustained decline in eGFR of at least 50%, ESKD, or death from renal or CV causes. Dapagliflozin reduced the risk of the primary outcome by 44% (HR, 0.56; 95% CI, 0.45 to 0.68) with a number needed to treat of 19 and an overall mortality benefit (HR, 0.69; 95% CI, 0.53 to 0.88). Importantly, 32.5% of patients enrolled did not have T2DM and 14.5% had an eGFR below 30 mL/min/1.73 m2, demonstrating the benefit of dapagliflozin across a range of kidney function regardless of diabetes status [47]. Please see Table 1 which summarizes the key findings. In addition to these completed trials, The Study of Heart and Kidney Protection With Empagliflozin (EMPA-KIDNEY, NCT03594110) is currently underway and is recruiting a broader group of participants with eGFRs as low as 20 mL/min/1.73 m2, without the requirement for albuminuria in patients with lower eGFR between 20 to 45 mL/min/1.73 m2. Therefore, this innovative and important trial design feature has the potential to extend the use of this class of medication to those with normo- or microalbuminuria—a subgroup of patients who have yet to be included in prior key kidney protection trials.
Beyond clinical kidney benefits, CVOT and kidney outcome trials have consistently demonstrated benefits on HF outcomes, leading to dedicated HF outcome trials. The Study to Evaluate the Effect of Dapagliflozin on the Incidence of Worsening Heart Failure or Cardiovascular Death in Patients With Chronic Heart Failure (DAPA-HF, NCT03036124) and Empagliflozin Outcome Trial in Patients With Chronic Heart Failure With Reduced Ejection Fraction (EMPEROR Reduced, NCT03057977) both demonstrated HF [48,49] and kidney benefits [50,51] in participants with HF and reduced ejection fraction with and without diabetes. Results of the Dapagliflozin Evaluation to Improve the Lives of Patients With Preserved Ejection Fraction Heart Failure (DELIVER, NCT03619213) and Empagliflozin Outcome Trial in Patients With Chronic Heart Failure With Preserved Ejection Fraction (EMPEROR Preserved, NCT03057-951) in participants with HF and preserved ejection fraction are awaited.
SGLT2 inhibition and safety
Overall, clinical trials have reported lower rates of total adverse events with SGLT2 inhibition [32,33,46]. A secondary analysis of CREDENCE showed no differences in the rate of adverse events when stratified by GFR [52]. Mycotic genital infections remain among the most common side effects while diabetic ketoacidosis is an uncommon but serious complication [53]. An increased risk of amputations was reported in the CANVAS Program trial but has not been demonstrated in any other clinical trial nor was there any signal of this issue in a meta-analysis involving 57,713 participants [54]. Similarly, despite theoretical concerns around an increased risk of acute kidney injury (AKI), SGLT2 inhibitors have been associated with lower rates of AKI, possibly due to prevention of ischemia in the kidney [55,56].
GLP-1 RAs, CARDIOVASCULAR AND RENAL PROTECTION IN PATIENTS WITH T2DM
GLP-1 RA and effects on metabolism
GLP-1 RAs increase insulin secretion, stimulate glucose uptake and delay gastric emptying, leading to significant reductions in glycated hemoglobin (HbA1c) and a greater likelihood of achieving an HbA1c of ≤7% [57]. GLP-1 RAs also increase self-reported post-prandial satiety, thereby reducing energy intake by 16% [58] and body weight by 2 to 4 kg [57]. Weight loss stems primarily from a reduction in body fat as opposed to lean mass and this weight change is sustained over long-term follow-up [59]. The mechanisms responsible for weight loss are in part due to GLP-1 RA effects on appetite and satiety control centers in the central nervous system [60].
GLP-1 RA and effects on natriuresis, blood pressure, and kidney function
Although GLP-1 receptors are found in CV tissues [61], the effect of GLP-1 RAs on CV physiological parameters such as blood pressure and heart rate is modest. In randomized controlled trials, GLP-1 RAs reduce systolic blood pressure by approximately 1 to 2 mm Hg, with lesser effects on diastolic blood pressure [62]. In addition, GLP-1 RAs did not reduce the incidence of new onset hypertension compared to placebo [62] and increased heart rate by 2 to 3 beats per minute compared to placebo [62]. Based on these modest effects, it is not clear if blood pressure lowering with GLP-1 RAs contributes mechanistically for improved cardiorenal outcomes with these agents in pivotal clinical trials (discussed below).
Beyond effects on blood pressure, glucose homeostasis and metabolism, GLP-1 RAs have additional effects on the kidney and CV system (see Table 1 for a summary of effects). In the kidney, GLP-1 receptors are located at the afferent arteriole [63] and proximal tubule [64], which leads to divergent acute effects on renal hemodynamics. For instance, in a non-randomized crossover study of healthy obese men who were administered exenatide, there was a 33% reduction in afferent arteriolar resistance and no change in efferent arteriolar resistance compared to placebo after a single dose [65]. The net effects were increases in renal blood flow and glomerular filtration rate [65]. Of interest, these renal hemodynamic changes were attenuated by concomitant administration of exenatide and the nitric oxide (NO)-synthase inhibitor L-NG-monomethyl arginine [65], a finding which has been confirmed in subsequent experimental studies [66]. These observations suggest that the effects of GLP-1 RAs at the afferent arteriole is in part mediated by NO.
In addition to effects on NO, GLP-1 RAs may impact other vasoactive mediators such as the renin-angiotensin-aldosterone system (RAAS). In a crossover study of healthy men who received a 2-hour infusion of synthetic human GLP-1, there was a 19% decrease in circulating angiotensin II levels, but no change in plasma levels of renin or aldosterone [67], and no alteration in renal hemodynamic function [67]. This decrease in circulating markers of the RAAS has not been consistently observed in human mechanistic studies, possibly due to differences in the study cohorts involved in these trials [68]. Further work is required to elucidate the relationship between GLP-1 RAs and neurohormonal activation, including the RAAS, and whether there are any implications for renal or systemic hemodynamic function, or clinical endpoints.
Through interactions with GLP-1 receptors in the proximal tubules, GLP-1 RAs also have natriuretic and diuretic effects. Administration of GLP-1 RA increases the fractional excretion of sodium and urine volume [65,67,69,70]. Natriuresis induced by GLP-1 RA likely result in large part from blockade of the sodium-hydrogen exchange transporter isoform 3 (NHE3) at the proximal tubule. In vitro, the GLP-1 agonist exendin-4, inhibits NHE3 through modulation of protein kinase A and cyclic adenosine monophosphate, culminating in downstream phosphorylation of the NHE3 transporter without changes in the surface expression within renal tubular cells [71]. This results in natriuretic effects [72] in a variety of animal models [73]. It would perhaps be anticipated that a proximal natriuresis should activate tubuloglomerular feedback at the macula densa, thereby causing afferent arteriolar vasoconstriction and a decrease in GFR. In contrast with this expected effect, eGFR does not change in patients with T2DM in response to GLP-1 RA in response to chronic treatment. First, in pivotal trials of GLP-1 RAs, there is no acute decrease in GFR that would be expected with proximal natriuresis, suggesting that there is minimal renal hemodynamic response to GLP-1 RAs. In the long-term, a meta-analysis of CVOTs of available GLP-1 RAs did not demonstrate a reduction in the incidence of worsening of kidney function (HR, 0.87; 95% CI, 0.73 to 1.03). However, to make matters more complex, there was moderate heterogeneity among the included trials, with an I2 of 43%. Notably, in the Researching Cardiovascular Events With a Weekly Incretin in Diabetes (REWIND) trial comparing dulaglutide to placebo, there was an 11% reduction in the incidence of a sustained decline in eGFR of ≥30% (HR, 0.89; 95% CI, 0.78 to 1.01) but further sensitivity analyses showed a 30% and 44% reduction in the incidence of a sustained decline of eGFR of ≥40% (HR, 0.70; 95% CI, 0.57 to 0.85) and ≥50% (HR, 0.56; 95% CI, 0.41 to 0.76) respectively [74]. The reason for modest, albeit highly variable, longer-term effects on GFR despite a proximal natriuresis is not known. Given the complex mechanisms at play, it may be that in the overall population of adults with diabetes, GLP-1 RAs have minimal effects on GFR but may be more beneficial within specific subpopulations.
Beyond effects on GFR, GLP-1 RAs reduce albuminuria. For instance, liraglutide and semaglutide were associated with a 26% reduction (HR, 0.74; 95% CI, 0.60 to 0.91) and 46% reduction (HR, 0.54; 95% CI, 0.37 to 0.77) in the incidence of new onset persistent macroalbuminuria compared to placebo in the Liraglutide Effect and Action in Diabetes: Evaluation of Cardiovascular Outcome Results (LEADER) and Trial to Evaluate Cardiovascular and Other Long-term Outcomes With Semaglutide in Subjects With Type 2 Diabetes (SUSTAIN-6) trials, respectively [75,76]. Likewise, dulaglutide was associated with a 23% reduction in new onset macroalbuminuria (HR, 0.77; 95% CI, 0.68 to 0.87) compared to placebo in the REWIND trial [74]. A Research Study to See How Semaglutide Works Compared to Placebo in People With Type 2 Diabetes and Chronic Kidney Disease (FLOW, NCT03819153) is currently recruiting, and its primary endpoint is a composite outcome defined as persistent eGFR decline of greater than or equal to 50%, reaching ESKD, death from kidney disease or death from CV disease.
The lack of a robust or consistent hemodynamic effect with GLP-1 RAs suggest that non-hemodynamic mechanisms could be responsible for the decline in albuminuria and possible eGFR preservation with these agents, including improvements in glucose control and metabolic parameters. Potential non-glycemic factors that may be kidney protective with GLP-1 RA include suppression of inflammatory pathways by preventing macrophage infiltration and decreasing oxidative stress [77], as reported in experimental models. Finally, reductions in body weight and blood pressure may also be beneficial, although the impact of these modest changes is less likely to be clinically relevant.
GLP-1 RA and effects on cardiovascular risk
From a CV perspective, GLP-1 RAs reduce CV risk compared to placebo in CVOTs. In a recent meta-analysis including all available CVOTs for GLP-1 RAs, all-cause mortality was reduced by 12% (HR, 0.88; 95% CI, 0.83 to 0.95), CV mortality by 12% (HR, 0.88; 95% CI, 0.81 to 0.96) and three-point MACE by 12% (HR, 0.82; 95% CI, 0.82 to 0.94) compared to placebo [78]. While there was moderate statistical heterogeneity for three-point MACE in these analyses, there was no evidence of subgroup differences based on the pharmacologic characteristics of studied agents or the baseline characteristics of adults enrolled in the clinical trials. Importantly, the benefits for MACE were consistent in adults with and without DKD.
Beyond effects on MACE and atherosclerosis, HF is an important source of morbidity and mortality in adults with diabetes. HF is in part characterized by myocardial insulin resistance, which contributes to impaired calcium uptake and mitochondrial function within the heart [79,80]. Therefore, agents that alter insulin sensitization or release have been theorized as possible treatments for these metabolic abnormalities seen in the setting of HF. In contrast with SGLT2 inhibitors, GLP-1 RAs have only a modest effect on the risk of HF hospitalization. For instance, in meta-analyses, GLP-1 RAs were associated with a 9% reduction in the incidence of HHF (HR, 0.91; 95% CI, 0.83 to 0.99) [78]. Likewise, for acute decompensated HF, there was no evidence of benefit with respect to HF re-hospitalization for liraglutide compared with placebo [81]. Therefore, combining GLP-1 RAs with SGLT2 inhibitors in clinical practice may be a strategy to leverage the benefits of each agent for MACE and HF respectively. Further research is needed to better ascertain the overall benefit-risk profile of this approach.
NON-STEROIDAL MINERALOCORTICOID RECEPTOR ANTAGONISTS, CARDIOVASCULAR AND KIDNEY PROTECTION IN PATIENTS WITH T2DM
The case for additional RAAS blockade in diabetic kidney disease
RAAS blockade is a pillar of DKD management, with benefits demonstrated in clinical trials for both primary and secondary prevention [82–86]. However, even when used in conjunction with SGLT2 inhibitors, patients with DKD continue to have significant residual risk of progression [46,47]. After success in trials with single agent RAAS blockade, interest shifted to dual RAAS blockade. The Ongoing Telmisartan Alone and in combination with Ramipril Global Endpoint trial (ONTARGET) was one of the earlier trials of dual RAAS blockade, randomizing 25,000 participants with vascular disease or diabetes to ramipril, telmisartan, or both. Dual therapy did reduce proteinuria to a greater extent, albeit in the context of increased rates of kidney function decline, dialysis, or death [87]. The Veteran Affairs-Diabetes in Nephropathy Study (VA-NEPHRON-D) and Aliskiren Trial in Type 2 Diabetes Using Cardiovascular and Renal Disease Endpoints (ALTITUDE) trials similarly assessed combination RAAS blockade but were discontinued early due to increased rates of hyperkalemia, AKI, and hypotension [88,89]. A role for mineralocorticoid receptor antagonism in DKD has been appealing with a strong physiological rationale, since mineralocorticoid receptors are widely expressed in kidney and cardiac tissue, and their activation by aldosterone leads to hemodynamic and non-hemodynamic effects culminating in inflammation, fibrosis, and progression of cardiac and kidney disease [90–97]. Until recently, clinical studies of MRA in CKD had not looked at ‘hard’ outcomes, although there is increased risk of hyperkalemia as demonstrated by a Cochrane review summarizing the literature up to but excluding Efficacy and Safety of Finerenone in Subjects With Type 2 Diabetes Mellitus and Diabetic Kidney Disease (FIDELIO-DKD) [98].
Novel mineralocorticoid receptor antagonists in diabetic kidney disease
Considering the uncertainty surrounding the use of traditional MRAs in CKD despite the establishment of their therapeutic role in HF with reduced ejection fraction, there has been growing interest in novel MRAs with higher selectivity, potency and with reduced risk of hyperkalemia [99]. FIDELIO-DKD was a phase 3 trial of finerenone, in addition to standard of care, in participants with T2DM, moderately advanced CKD (mean baseline eGFR was 44 mL/min/1.73 m2 with a median UACR of 852 mg/g) with the majority (87%) having macroalbuminuria [100]. The primary outcome was a composite kidney outcome—kidney failure, sustained ≥40% decline in eGFR, or death from renal causes. A secondary composite kidney outcome identical to the primary outcome but with a 57% decline in eGFR was also included. Finerenone significantly reduced the incidence of the primary and secondary kidney outcomes by 18% and 24% respectively, with a number needed to treat of 29 patients for the primary outcome. Breaking down the components of kidney composite outcomes, finerenone reduced the ≥57% decline in eGFR outcome by 32% (95% CI, 0.55 to 0.82), and the kidney failure/ESKD by 13% (95% CI, 0.72 to 1.05). Examining the between-group eGFR differences, after considering a finerenone associated acute decline in eGFR of 2.5 mL/min/1.73 m2 compared to placebo, the finerenone group declined by 2.66 mL/min/1.73 m2/year versus a 3.97 mL/min/1.73 m2/year decline in the placebo group, with a crossing of the eGFR curves occurring at approximately 24 months. Finerenone additionally reduced UACR by 31% versus placebo within the first 4 months (95% CI, 0.66 to 0.71) and onwards, and was associated with small reductions in blood pressure (Table 1).
In keeping with established links between kidney and CV health, finerenone also reduced rates of the CV outcome compared to placebo, an effect that was apparent within a month of starting the study drug [100]. Results of the ongoing Efficacy and Safety of Finerenone in Subjects With Type 2 Diabetes Mellitus and the Clinical Diagnosis of Diabetic Kidney Disease (FIGARO-DKD, NCT02545049) trial can be expected to shed further light on CV and HF outcomes.
Non-steroidal mineralocorticoid receptor antagonists and safety
FIDELIO-DKD did not show an increase in the anticipated adverse events including AKI, breast hyperplasia, or gynecomastia. While finerenone increased the risk of hyperkalemia, the risk of it leading to study drug discontinuation was low (2.3% with finerenone compared to 0.9% with placebo). Additionally, this rate of study drug discontinuation was numerically lower compared to rates in prior studies of dual RAAS inhibition (ALTITUDE 4.8% and VA-NEPHRON-D 9.9%). Finerenone also appears to be safer than steroidal MRAs as demonstrated in the ARTS trial where several doses were compared to spironolactone and placebo [101]. While increases in serum potassium levels were observed compared to placebo, the increase was significantly lower compared to spironolactone at all doses of finerenone.
COMBINED USE OF NOVEL AGENTS FOR THE TREATMENT OF DKD
SGLT2 inhibitors, GLP-1 receptor agonists and non-steroidal MRAs are expected to be increasingly used together in the setting of DKD on a background of single agent RAAS blockade. Studies examining the use of these agents together in the setting of clinical trials, real world analyses, or mechanistic trials will be important to characterize the nature of their combined heart and kidney benefits. There is some data on the combined use of SGLT2 inhibitors and GLP-1 receptor agonists. The 28-week, phase three, Evaluate Efficacy and Safety of Exenatide Once Weekly and Dapagliflozin Versus Exenatide and Dapagliflozin Matching Placebo (DURATION-8) trial demonstrated that dual therapy with dapagliflozin and exenatide had additive effects on lowering weight and blood pressure, though with a less than additive effect on HbA1c [102]. Additive effects on weight loss were similarly demonstrated in the Efficacy and Safety of Semaglutide Once-weekly Versus Placebo as add-on to SGLT-2i in Subjects With Type 2 Diabetes Mellitus (SUSTAIN-9) and Dulaglutide as add-on therapy to SGLT2 inhibitors in patients with inadequately controlled type 2 diabetes (AWARD-10) trials [103,104]. The effect of such combination therapy on heart and kidney outcomes in DKD is unknown, though it is conceivable that additive benefits on weight loss and blood pressure would confer additive benefits on harder clinical outcomes (Table 1). A propensity-matched cohort from the Exenatide Study of Cardiovascular Event Lowering Trial (EXSCEL) trial demonstrated that the addition of exenatide in patients on a background of SGLT2 inhibition resulted in modest improvements in MACE, all-cause mortality and slower rates of renal decline compared to patients not on an SGLT2 inhibitor [105]. Results of the FLOW trial (NCT03819153) are also anticipated as a larger proportion of participants will be expected to be on concomitant SGLT2 inhibition. Based on the study design of FIDELIO-DKD, finerenone is intended to be used as add-on therapy to ACE inhibition or ARBs, and only a small proportion of participants were treated with SGLT2 inhibition due to the era of the trial. There additionally exists a safety argument for using MRAs in combination with SGLT2 inhibitors to reduce the risk of hyperkalemia, since the latter medication class has a modest potassium lowering effect as suggested by a recent post hoc analysis of MRA use in DAPA-HF [106]. Only 4% to 11% of FIDELIO-DKD participants were on an SGLT2 inhibitor over the course of the study, and CREDENCE did not enroll participants taking an MRA at baseline, so there is limited evidence for the combined use of these two agents currently. See Fig. 1 regarding the possible sequential or combined use of these three classes of medications, starting with the areas of strongest evidence.
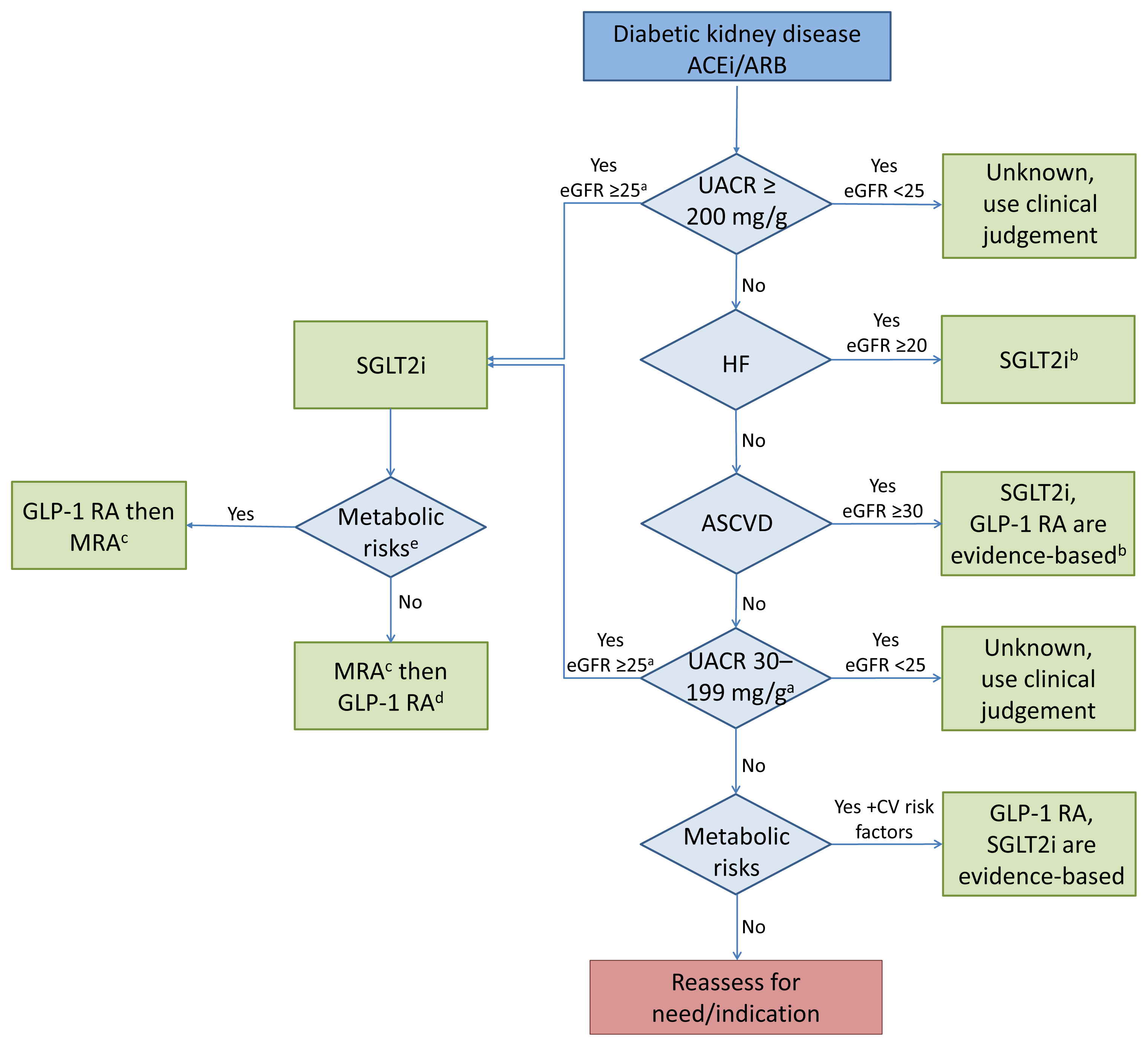
Decision algorithm for prescribing sodium-glucose cotransporter-2 inhibitor (SGLT2i), glucagon-like peptide-1 receptor agonist (GLP-1 RA) and mineralocorticoid receptor antagonist (MRA) to optimize heart and kidney protection in patients with diabetic kidney disease. ACEi, angiotensin converting enzyme inhibitor; ARB, angiotensin receptor blocker; UACR, urinary albumin-to-creatinine ratio; HF, heart failure; ASCVD, atherosclerotic cardiovascular disease. aEMPA KIDNEY trial may allow use of SGLT2i down to eGFR of 20 without albuminuria; bFIGARO trial in progress which will give further information on use of MRA in HF and ASCVD; cAdd on if residual albuminuria with UACR >30 mg/g despite optimal medical therapy; dFLOW trial may suggest GLP-1 RA use to prevent composite renal outcome; eMetabolic risk, poor glycemic control or weight loss desired.
CONCLUSIONS
The management of DKD has evolved over the last 5 years with a renewed emphasis on therapeutic agents associated with heart and kidney protection. SGLT2 inhibitors have established benefits on kidney, CV and HF outcomes in the setting of DKD. GLP-1 RA therapies have also been noted to have heart and kidney protective effects, although benefits in the kidney at this time appear to be isolated to preventing the progression of proteinuria, and CV benefits appear to be primarily anti-atherosclerotic rather than on the basis of preventing HHF with SGLT2 inhibitors. Finally, non-steroidal MRAs are the latest addition to the DKD armamentarium with evidence of kidney and CV benefits. Further work is required to determine the impact of combinations of these therapies on heart and kidney endpoints in patients with diabetes.
Acknowledgements
Vikas S. Sridhar is supported by the Department of Medicine Eliot Phillipson Clinician Scientist Training Program and a Banting and Best Diabetes Centre Postdoctoral fellowship at the University of Toronto. David Z.I. Cherney is supported by a Department of Medicine, University of Toronto Merit Award and receives support from the CIHR, Diabetes Canada and the Heart and Stroke Richard Lewar Centre of Excellence.
Notes
CONFLICTS OF INTEREST
David Z.I. Cherney has received honoraria from Boehringer Ingelheim-Lilly, Merck, AstraZeneca, Sanofi, Mitsubishi-Tanabe, Abbvie, Janssen, Bayer, Prometic, BMS, Maze and Novo-Nordisk and has received operational funding for clinical trials from Boehringer Ingelheim-Lilly, Merck, Janssen, Sanofi, AstraZeneca and Novo-Nordisk. Others have no conflicts of interest to declare.