Riedel Thyroiditis in a Patient with Graves Disease
Article information
Abstract
Riedel's thyroiditis is a rare form of infiltrative and inflammatory disease of the thyroid gland and can be associated with systemic fibrotic processes, Hashimoto thyroiditis and Graves disease. Riedel thyroiditis in combination with Graves disease however, is very rare. A 57-year-old woman with a past medical history significant for Graves disease diagnosed 30 years ago presented with an enlarging neck mass and voice changes. Due to suspicion of malignancy, thyroidectomy was performed. Histopathologic examination revealed Riedel thyroiditis. To our knowledge, the association of Riedel thyroiditis with Graves disease has not yet been reported in our country. Here we report a patient with Riedel thyroiditis evolved from antecedent Graves disease.
INTRODUCTION
Riedel thyroiditis (RT) is a rare form of infiltrative and fibrotic disease of the thyroid. It is characterized by breathing difficulties and dysphagia resulting from pressure from a rapidly enlarging thyroid. In rare cases, it can cause voice hoarseness if the enlarged thyroid damages the recurrent laryngeal nerve. Riedel [1] first recognized the disease in 1896. The cause of RT is not yet clear, but an immune disorder is considered the most likely cause [2,3]. Recent research has shown that immunoglobulin G4-related systemic disease (IgG4-RSD) is likely involved [4-9]. In 1985, Hay et al. [10] reported that RT was identified in 30 of 5,700 cases of thyroidectomy during the period from 1920 through 1984, according to histopathologic examination at the Mayo Clinic. The incidence rate was estimated at 0.06 to 1.06 per 100,000 people. In their study, the number of female patients with RT was three times higher than the number of men, and the median age of female patients was 51 years. Of 37 patients with RT, 12 experienced fibrosclerosis of the cervix, mediastinum, or retroperitoneum within 10 years after thyroidectomy [10].
Pi et al. [11] reported a case study in which a thyroidectomy was recommended for a patient with RT that was difficult to differentiate from thyroid cancer. However, no case of concurrent RT and Graves disease has been reported in the local literature. The authors diagnosed RT in a 57-year-old woman with Graves disease who presented with paralyzed vocal cords. Herein, we present a case of RT cured with surgical treatment, and a review of the literature.
CASE REPORT
Patient
Mrs. Kim, age 57.
Chief complaint
Recently enlarging neck mass and hoarseness that started 5 days before admission to the hospital.
Present medical condition
A 57-year-old woman visited the outpatient clinic with a very hard, fixed lump that had been present on the right side of her neck for months and hoarseness, which started 5 days previous. The patient had previously taken antithyroid agents prescribed by a private hospital but did not undergo additional tests or follow-up related to her hyperthyroidism. She did not show any symptoms associated with thyrotoxicosis on admission.
Past medical history
She underwent intermittent treatment for hyperthyroidism over the last three decades. She has had no other symptoms.
Family medical history
No medical problems.
Physical examination
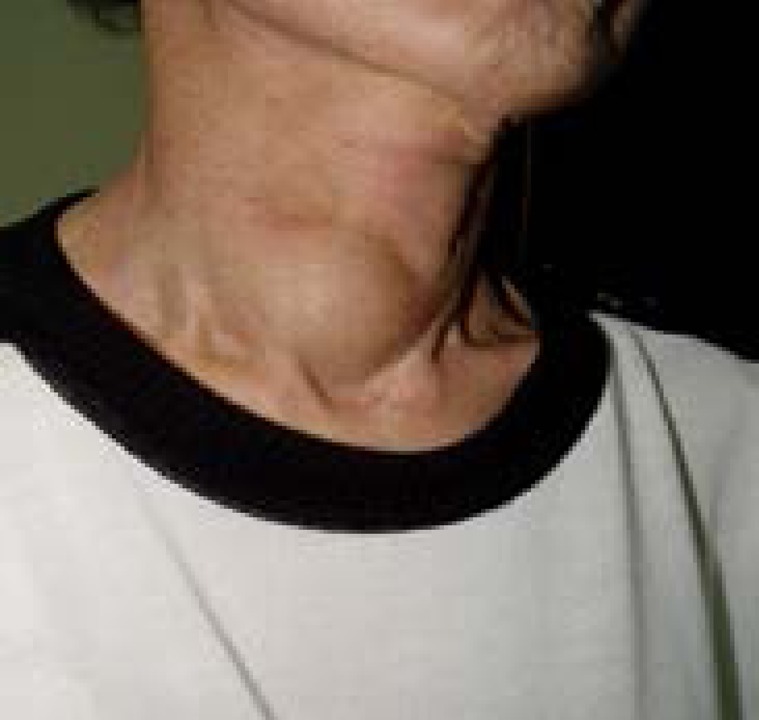
The patient was conscious and in no acute distress. She was medically stable with a blood pressure of 130/90 mm Hg, pulse of 76 beats per minute, respiration rate of 20 breaths per minute, and a temperature of 36.5℃. Globe protrusion, scleral icterus, and conjunctival anemia were not observed. Enlarged cervical lymph nodes and jugular vein engorgement were also not present. A hard and fixed thyroid nodule that measured approximately 5×4 cm was palpated, but no neck tenderness was appreciated (Fig. 1). On auscultation, normal heart and breath sounds were observed. Physical examination revealed no pitting edema in her extremities.
Lab results
Complete blood count revealed a white blood cell count of 6,460/mm3 (neutrophil 57.4%, lymphocyte 36.6%, monocyte 7.7%, eosinophil 0.6%), hemoglobin of 11.6 g/dL, hematocrit of 35.2%, and platelet count of 295×103/mm3. Urine test was normal. Serum biochemical examination revealed a blood urea nitrogen/creatinine of 25/0.6 mg/dL, total protein/albumin of 7.4/4.3 g/dL, aspartate aminotransferase/alanine aminotransferase of 22/20 IU/L, Na/K/Cl of 142/5.1/105 mEq/L, Ca of 4.6 mEq/L (normal range, 4.5 to 5.2), erythrocyte sedimentation rate of 19 mm/hr, and C-reactive protein <0.2 mg/day. Thyroid function tests revealed thyroid stimulation hormone of 0.07 µIU/mL (normal range, 0.4 to 4.5), free T4 of 3.86 ng/dL (normal range, 0.7 to 2), TBII of 51% (normal range, 0 to 15), thyroglobulin of 493 ng/dL (normal range, 2 to 60), antithyroid microsomal antibody of 3.1 U/mL (normal range, 0 to 8), and negative thyroglobulin antibody of 22 U/mL (normal range, 0 to 55), consistent with Graves disease.
Electrocardiography
Normal sinus rhythm.
Chest radiography
Signs of emphysema and right to left shift of the trachea as a consequence of the thyroid nodule.
Thyroid ultrasound
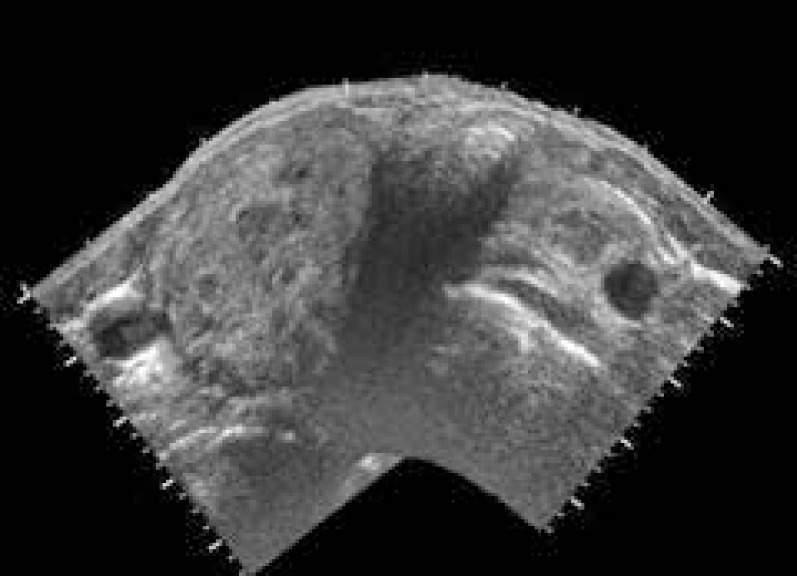
A well-defined irregular and hypoechoic nodule measuring 4 cm in diameter, along with large scattered dense calcifications, was observed in the right thyroid lobe (Fig. 2). However, enlarged cervical lymph nodes and invasion into the parathyroid glands were not present.
Thyroid fine needle aspiration (FNA) cytology
Since repeated nonaspiration technique failed to obtain a specimen, we employed an aspiration technique which yielded a very small amount of cytologic specimen. In cytopathologic examination, no malignant cells were detected, but adenomatous goiter was suspected. Although thyroid cancer was not diagnosed by FNA, the large, solid mass and paralyzed vocal cords on the right side suggested the possibility of thyroid cancer. Therefore, a surgical approach was determined for histological diagnosis and treatment.
Computed tomography (CT) scan of the neck
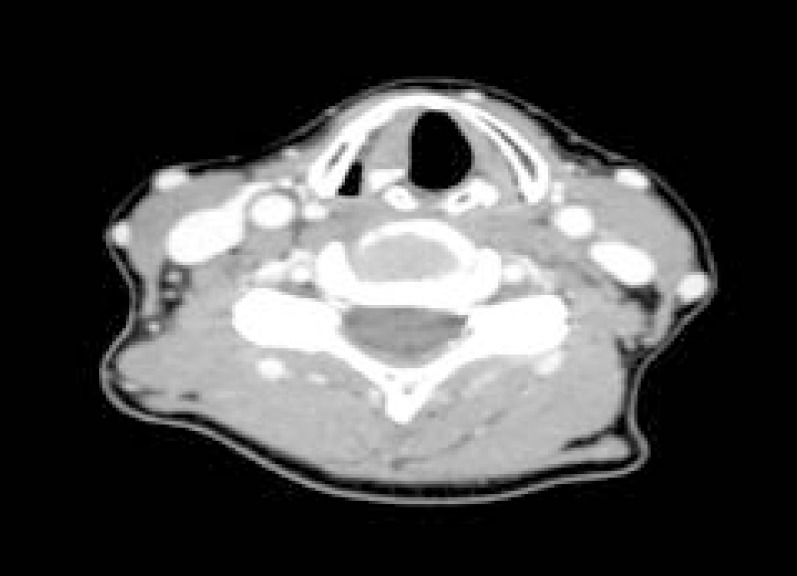
There was a 4.3×4.0 cm nodular lesion occupying most of the right lobe of the thyroid. A peripheral calcified lesion was also identified. Very severe marginal calcification was detected in the inferior portion of the nodule, which was barely observable in ultrasonography (Fig. 3). Unilateral fixed vocal cords were revealed in a paramedian position. Vocal cord paralysis was suspected on the right side (Fig. 4).
Surgery
A total thyroidectomy was performed. A 4.5-cm solid mass of the right thyroid lobe was closely adhered to the surrounding airway and recurrent laryngeal nerve. It was impossible to completely dissect the mass from the nerve.
Histological examination
The resected mass was covered by a thin capsule, and its cut surface showed mixed strips of white, yellowish-brown, and pink colors. Peripheral dense calcification was also seen. Microscopic examination revealed that thyroid follicles were replaced by extensive inflammatory and fibrous tissue. Inflammation was also noticed in the vein, which was encased in fibrous tissue, but no malignant cells were found. Based on these pathologic characteristics, RT was diagnosed (Fig. 5).

(A) Enlarged right lobe of the thyroid with calcification. (B) Extensively hyalinized fibrous tissue replaced the thyroid gland. Fibrosis and inflammation extended beyond the thyroid capsule (H&E stain, ×100). (C) Medium-sized veins encased by fibrosis indicating inflammation of their walls. The inflammation is of the monocuclear type, with a predominance of lymphocytes (H&E stain, ×400).
Outcome
The patient recovered from RT, and there were no signs of complications. She is currently taking 100 µg levothyroxine while undergoing postsurgical outpatient follow-up. She has not yet recovered from her vocal cord paralysis.
DISCUSSION
RT is a very unusual form of thyroid disease, characterized by extensive fibrosis of the thyroid tissue [1]. RT was first recognized as one type of inflammatory thyroiditis, but it is increasingly seen as a distinct disease associated with autoimmune disorders and systemic multifocal fibrosclerosis. The hypothesis of an association between RT and an autoimmune mechanism has several supportive findings [4]; for example, thyroid-specific autoantibodies have been detected in many patients with RT; RT occurs in conjunction with other autoimmune diseases such as Hashimoto thyroiditis, Graves disease, and pernicious anemia; infiltration with lymphocytes, plasma cells, and histiocytes is often evident in RT; local vasculitis is commonly found on pathology; and lastly, RT responds well to systemic steroids. On the other hand, RT was not considered an autoimmune disease in some studies for the following reasons: the lymphocyte subpopulation of white blood cells and serum complement levels are usually normal, and the increase in thyroid antibody may be a response elicited by antigens in thyroid tissue.
Systemic multifocal fibrosclerosis is a syndrome characterized by fibrosis involving various organs, including those of the retroperitoneum and mediastinum, the orbit, lung, bile duct, lacrimal gland, and parotid gland. In several studies, RT was regarded as one clinical symptom of multifocal fibrosclerosis [4-6]. Particularly, Fatourechi et al. [7] reported that 38% of patients with RT showed a fibrotic process that extended beyond the neck. Recent studies have claimed that RT is more likely associated with multifocal fibrosclerosis and IgG4-RSD. IgG4-RSD is a disease in which a mass may be formed by inflammatory activation of IgG4-positive plasma cells that are related to fibrosclerosis and obliterative phlebitis [8]. RT is considered a type of multifocal fibrosclerosis seen in IgG4-RSD due to its immunohistochemical profile [9]. Heufelder and Hay [12] reported the incidence of RT in patients with Graves disease, and McIver et al. [13] discussed Graves disease in patients with unilateral RT. In the latter study, Graves disease occurred within 3 years after RT stabilization, indicating the important role of an autoimmune mechanism in causing RT. This case study also suggests the involvement of an autoimmune mechanism in RT because the patient had medical history of hyperthyroidism over the last three decades and Graves disease on admission.
Most patients with RT are admitted to the hospital because of a rapidly enlarging goiter and its pressure on surrounding tissue. Thyroid nodules extend to both lobes in most cases, are solid like a stone, and are fixed as a result of invasion and adhesion to surrounding tissue. The pressure that the enlarged thyroid puts on surrounding structures causes shortness of breath, dysphagia, suffocation, and hoarseness. The differential diagnoses include thyroid cancer, thyroid lymphoma, and Hashimoto thyroiditis. However, fibrotic proliferation to surrounding tissue is not common in these diseases. Lab results in RT are usually nonspecific; most patients with these diseases maintain normal thyroid function. According to Cleveland Clinic's report, 64% of total patients had normal thyroid function, 32% had hypothyroidism, and 4% had hyperthyroidism [2]. Nearly 45% to 67% of patients were positive for antithyroid antibody, but the titer of antibody was lower than that in patients with Hashimoto thyroiditis.
RT is a very rare disease, and its clinical characteristics are not easily differentiated from those of thyroid carcinoma, primary thyroid lymphoma, and undifferentiated carcinoma. The final diagnosis therefore depends on histological findings. As Harigopal et al. [14] suggested, RT can be diagnosed based on triplicated findings of FNA performed with an adequate amount of specimen, physical examination, antibody test, and radiological test. However, obtaining adequate amount of specimen necessary for testing is not easy in FNA and core needle biopsy. Also, suspicious cells may be found in collected tissues. Therefore, surgical biopsy is usually performed instead of these methods. In this study, thyroid cancer was suspected based on radiological imaging, while FNA revealed only adenomatous goiter. A thyroidectomy was performed for histological diagnosis and treatment. In thyroidectomy, the dissection process is often very difficult as the fibrotic mass can extend to the bronchus, cervical muscle, esophagus, and nerve plexus. The thyroid frequently is hard like cartilage and does not have blood vessels, so it often does not bleed during dissection. In this study, the dissection was difficult as the mass was adhered to the airway and recurrent laryngeal nerve.
It is important to differentiate characteristics of RT from those of Hashimoto thyroiditis. Along with fibrosis of thyroid tissue, fibrosis of surrounding structures and obstructive phlebitis differentiates RT from characteristics of Hashimoto thyroiditis. In terms of immunohistochemical profile, overall fibrosis and infiltration with granulocytes, monocytes, and eosinophils are more severe in RT, while fibrosis with histiocytes and CD8+ T&B lymphocytes is less severe compared to Hashimoto [15]. Harach and Williams [16] presented differences between RT and Hashimoto's using immunohistochemical staining. According to their study results, RT contained a greater number of λ-IgA in histiocytes, while Hashimoto showed a greater number of κ-IgG [16]. Although differences between RT and Hashimoto are identifiable through clinical, histological, and immunological tests, caution is needed to obtain the proper diagnosis.
Radiological evaluation of RT is nonspecific. Although image scans show decreased thyroid uptake and an inhomogeneous pattern in RT, other kinds of thyroiditis can also present this way. RT is seen on ultrasound as an irregular and hypoechoic lesion due to extensive fibrosis. A CT scan is the best test to confirm the invasion of the mass to surrounding organs. In CT imaging, a lesion appears hypodense, but the lesion's density is reinforced after the administration of contrast agent. A lesion appears low signal intensity in T1 and T2-weighted magnetic resonance imaging [17].
Most RT cases have good outcome. Mortality rarely occurs as a result of complications such as pneumonia and breathing difficulties caused by the pressure of the enlarged mass on the trachea.
Small-scale studies and case reports have been conducted to address the effects of drug treatment on RT, reporting good outcomes with the use of corticosteroids [12,18]. This medicine proved to be effective as early treatment in life-threatening extending fibrosis. Treatment with corticosteroids often takes a long-term course as symptoms often get worse after the drug is stopped. The antiestrogen tamoxifen is also effective in restraining the expansion of connective tissue. A study achieved good outcomes after using tamoxifen in a patient with progressive RT, although the patient took corticosteroids after surgery [19,20]. The mechanism of tamoxifen is unknown, but it appears to be related to transforming growth factor-β stimulation, which suppresses immature fibroblast and epithelial cells.
A surgical treatment is required when tissue sample is necessary for diagnosis, drug therapy fails, and pressure symptom is severe. A wedge resection in isthmic portion of the thyroid enables the surgeon to obtain tissue while separating the left and right lobes and easing pressure. Since the dissection of a mass is not easy due to adhesion to surrounding tissue, any extensive surgery such as subtotal or total thyroidectomy is not recommended.
This study presents a case of RT diagnosed in a woman who had treatment for hyperthyroidism over the last three decades and Graves disease on admission. The solid and fixed mass accompanied by hoarseness did not rule out the risk of thyroid cancer; so, a thyroidectomy was performed and RT was diagnosed. Concurrent RT and Graves disease is rare and herein reported for the first time in South Korea. In conclusion, we report important effects of an autoimmune mechanism on the onset of RT with clinical, radiological, and histological findings in the patient with concurrent RT and Graves disease.
In summary, we present a case of a 57-year-old woman who was admitted to our hospital with a solid thyroid mass accompanied by paralysis of the recurrent laryngeal nerve on the right side. She had received intermittent treatment for Graves disease for three decades. Since her clinical characteristics suggested a possible risk of thyroid cancer, a thyroidectomy was performed, and RT was diagnosed. We report her clinical characteristics and a review of the literature and emphasize the need for including RT in the differential diagnosis of autoimmune thyroid diseases presenting with a hard nodule.
Notes
No potential conflict of interest relevant to this article was reported.